Business Name: BeeHive Homes of Enchanted Hills
Address: 6336 Enchanted Hills Blvd NE, Rio Rancho, NM 87144
Phone: (505) 221-6400
BeeHive Homes of Enchanted Hills
BeeHive Homes of Enchanted Hills offers Assisted Living for your loved ones. 24x7 care in the comfort of a private room with bath. Meals are family style and cooked fresh each day. Stop by today and visit, and see why we always say "Welcome Home!
6336 Enchanted Hills Blvd NE, Rio Rancho, NM 87144
Business Hours
Monday thru Sunday: 9:00am to 5:00pm
Instagram: https://www.instagram.com/beehivehomesriorancho/
YouTube: https://www.youtube.com/@WelcomeHomeBeeHiveHomes
TikTok: https://www.tiktok.com/@beehivehomesriorancho
Families hardly ever plan for the moment a parent or partner requires more help than home can fairly provide. It creeps in silently. Medication gets missed out on. A pot burns on the stove. A nighttime fall goes unreported till a next-door neighbor notices a contusion. Selecting between assisted living and memory care is not just a real estate decision, it is a clinical and emotional choice that impacts dignity, safety, and the rhythm of every day life. The expenses are substantial, and the differences among neighborhoods can be subtle. I have actually sat with households at kitchen tables and in medical facility discharge lounges, comparing notes, cleaning up myths, and translating jargon into genuine scenarios. What follows reflects those discussions and the practical realities behind the brochures.
What "level of care" actually means
The expression sounds technical, yet it comes down to how much help is needed, how frequently, and by whom. Neighborhoods assess locals throughout common domains: bathing and dressing, movement and transfers, toileting and continence, eating, medication management, cognitive support, and threat habits such as roaming or exit-seeking. Each domain gets a rating, and those scores connect to staffing requirements and regular monthly fees. Someone might need light cueing to remember an early morning regimen. Another might need two caregivers and a mechanical lift for transfers. Both could reside in assisted living, but they would fall under extremely different levels of care, with rate differences that can go beyond a thousand dollars per month.
The other layer is where care occurs. Assisted living is created for people who are primarily safe and engaged when given intermittent assistance. Memory care is built for people living with dementia who need a structured environment, specialized engagement, and staff trained to redirect and distribute anxiety. Some needs overlap, however the programs and security functions vary with intention.
Daily life in assisted living
Picture a studio apartment with a kitchen space, a personal bath, and adequate area for a favorite chair, a couple of bookcases, and household pictures. Meals are served in a dining room that feels more like an area cafe than a medical facility snack bar. The goal is self-reliance with a safety net. Staff help with activities of daily living on a schedule, and they check in between jobs. A resident can go to a tai chi class, sign up with a conversation group, or skip it all and checked out in the courtyard.
In useful terms, assisted living is a good fit when an individual:
- Manages most of the day independently however needs trustworthy help with a few tasks, such as bathing, dressing, or handling intricate medications. Benefits from prepared meals, light housekeeping, transport, and social activities to decrease isolation. Is normally safe without constant guidance, even if balance is not ideal or memory lapses occur.
I remember Mr. Alvarez, a previous store owner who relocated to assisted living after a small stroke. His daughter stressed over him falling in the shower and avoiding blood slimmers. With set up early morning help, medication management, and night checks, he discovered a new routine. He ate much better, gained back strength with onsite physical treatment, and quickly felt like the mayor of the dining-room. He did not need memory care, he needed structure and a team to identify the little things before they ended up being big ones.
Assisted living is not a nursing home in mini. Many communities do not use 24-hour licensed nursing, ventilator assistance, or complex wound care. They partner with home health companies and nurse professionals for intermittent experienced services. If you hear a guarantee that "we can do everything," ask particular what-if questions. What if a resident needs injections at accurate times? What if a urinary catheter gets blocked at 2 a.m.? The best neighborhood will answer plainly, and if they can not offer a service, they will tell you how they handle it.
How memory care differs
Memory care is developed from the ground up for individuals with Alzheimer's illness and associated dementias. Layouts decrease confusion. Hallways loop instead of dead-end. Shadow boxes and personalized door signs help citizens acknowledge their spaces. Doors are protected with quiet alarms, and courtyards permit safe outside time. Lighting is even and soft to reduce sundowning triggers. Activities are not just scheduled events, they are therapeutic interventions: music that matches an era, tactile tasks, guided reminiscence, and short, predictable regimens that lower anxiety.
A day in memory care tends to be more staff-led. Rather of "activities at 2 p.m.," there is a constant cadence of engagement, sensory cues, and mild redirection. Caretakers frequently understand each resident's life story well enough to connect in moments of distress. The staffing ratios are higher than in assisted living, due to the fact that attention requires to be ongoing, not episodic.
Consider Ms. Chen, a retired instructor with moderate Alzheimer's. In the house, she woke at night, opened the front door, and strolled up until a next-door neighbor assisted her back. She dealt with the microwave and grew suspicious of "complete strangers" going into to help. In memory care, a team rerouted her throughout uneasy periods by folding laundry together and walking the interior garden. Her nutrition improved with small, frequent meals and finger foods, and she rested much better in a quiet room far from traffic noise. The change was not about giving up, it had to do with matching the environment to the method her brain now processed the world.
The middle ground and its gray areas
Not everyone needs a locked-door unit, yet basic assisted living may feel too open. Lots of neighborhoods acknowledge this gap. You will see "boosted assisted living" or "assisted living plus," which typically suggests they can supply more regular checks, specialized behavior support, or higher staff-to-resident ratios without moving somebody to memory care. Some provide little, secure areas adjacent to the primary building, so locals can participate in performances or meals outside the community when suitable, then return to a calmer space.
The boundary usually boils down to respite care safety and the resident's response to cueing. Periodic disorientation that fixes with gentle pointers can typically be handled in assisted living. Consistent exit-seeking, high fall risk due to pacing and impulsivity, unawareness of toileting requires that leads to regular mishaps, or distress that intensifies in hectic environments often signals the requirement for memory care.
Families sometimes postpone memory care because they fear a loss of liberty. The paradox is that numerous citizens experience more ease, because the setting reduces friction and confusion. When the environment anticipates needs, self-respect increases.
How communities identify levels of care
An evaluation nurse or care organizer will fulfill the prospective resident, review medical records, and observe mobility, cognition, and habits. A couple of minutes in a quiet workplace misses crucial details, so excellent assessments consist of mealtime observation, a walking test, and a review of the medication list with attention to timing and side effects. The assessor must inquire about sleep, hydration, bowel patterns, and what happens on a bad day.
Most communities cost care utilizing a base rent plus a care level cost. Base lease covers the home, utilities, meals, housekeeping, and programs. The care level includes costs for hands-on assistance. Some service providers use a point system that transforms to tiers. Others use flat bundles like Level 1 through Level 5. The distinctions matter. Point systems can be accurate however fluctuate when needs change, which can annoy households. Flat tiers are predictable but may mix really various needs into the same price band.
Ask for a composed explanation of what qualifies for each level and how frequently reassessments happen. Also ask how they deal with temporary modifications. After a medical facility stay, a resident may need two-person support for two weeks, then return to standard. Do they upcharge immediately? Do they have a short-term ramp policy? Clear responses assist you budget and avoid surprise bills.
Staffing and training: the crucial variable
Buildings look gorgeous in pamphlets, however day-to-day life depends upon the people working the floor. Ratios differ commonly. In assisted living, daytime direct care coverage often ranges from one caretaker for eight to twelve homeowners, with lower protection overnight. Memory care often aims for one caretaker for six to eight homeowners by day and one for 8 to 10 in the evening, plus a med tech. These are detailed varieties, not universal rules, and state policies differ.
Beyond ratios, training depth matters. For memory care, try to find ongoing dementia-specific education, not a one-time orientation. Methods like recognition, positive physical technique, and nonpharmacologic habits techniques are teachable skills. When an anxious resident shouts for a partner who died years earlier, a well-trained caretaker acknowledges the feeling and offers a bridge to convenience rather than correcting the facts. That type of skill protects dignity and lowers the need for antipsychotics.
Staff stability is another signal. Ask how many company workers fill shifts, what the yearly turnover is, and whether the exact same caretakers normally serve the very same homeowners. Continuity builds trust, and trust keeps care on track.
Medical support, therapy, and emergencies
Assisted living and memory care are not hospitals, yet medical needs thread through daily life. Medication management prevails, consisting of insulin administration in lots of states. Onsite doctor check outs vary. Some neighborhoods host a going to medical care group or geriatrician, which lowers travel and can catch changes early. Numerous partner with home health suppliers for physical, occupational, and speech treatment after falls or hospitalizations. Hospice teams frequently work within the neighborhood near the end of life, permitting a resident to remain in location with comfort-focused care.
Emergencies still occur. Inquire about response times, who covers nights and weekends, and how staff intensify concerns. A well-run building drills for fire, severe weather condition, and infection control. Throughout breathing virus season, look for transparent communication, versatile visitation, and strong procedures for isolation without social overlook. Single spaces help reduce transmission however are not a guarantee.
Behavioral health and the difficult minutes families rarely discuss
Care needs are not just physical. Stress and anxiety, anxiety, and delirium make complex cognition and function. Discomfort can manifest as hostility in somebody who can not describe where it hurts. I have actually seen a resident identified "combative" relax within days when a urinary tract infection was treated and an inadequately fitting shoe was changed. Great communities operate with the presumption that behavior is a form of interaction. They teach staff to search for triggers: hunger, thirst, dullness, sound, temperature shifts, or a congested hallway.
For memory care, pay attention to how the team talks about "sundowning." Do they change the schedule to match patterns? Deal peaceful tasks in the late afternoon, modification lighting, or supply a warm treat with protein? Something as regular as a soft throw blanket and familiar music throughout the 4 to 6 p.m. window can alter a whole evening.
When a resident's requirements exceed what a community can safely deal with, leaders ought to discuss alternatives without blame: short-term psychiatric stabilization, a higher-acuity memory care, or, sometimes, a proficient nursing center with behavioral know-how. Nobody wishes to hear that their loved one needs more than the present setting, but prompt shifts can prevent injury and restore calm.
Respite care: a low-risk way to try a community
Respite care offers a supplied apartment or condo, meals, and full participation in services for a brief stay, generally 7 to thirty days. Households use respite during caretaker holidays, after surgical treatments, or to check the fit before committing to a longer lease. Respite remains expense more each day than basic residency because they include versatile staffing and short-term arrangements, but they provide vital data. You can see how a parent engages with peers, whether sleep improves, and how the team communicates.
If you are uncertain whether assisted living or memory care is the better match, a respite duration can clarify. Personnel observe patterns, and you get a reasonable sense of life without locking in a long contract. I often encourage families to schedule respite to start on a weekday. Complete groups are on website, activities perform at complete steam, and doctors are more offered for fast changes to medications or treatment referrals.
Costs, agreements, and what drives cost differences
Budgets form options. In numerous regions, base rent for assisted living varies commonly, typically starting around the low to mid 3,000 s per month for a studio and increasing with home size and area. Care levels add anywhere from a few hundred dollars to several thousand dollars, connected to the intensity of support. Memory care tends to be bundled, with all-inclusive rates that starts higher due to the fact that of staffing and security requirements, or tiered with fewer levels than assisted living. In competitive urban areas, memory care can start in the mid to high 5,000 s and extend beyond that for intricate needs. In suburban and rural markets, both can be lower, though staffing deficiency can push costs up.
Contract terms matter. Month-to-month agreements provide flexibility. Some communities charge a one-time community charge, typically equal to one month's lease. Ask about annual increases. Common range is 3 to 8 percent, but spikes can take place when labor markets tighten. Clarify what is included. Are incontinence products billed separately? Are nurse assessments and care strategy conferences constructed into the charge, or does each visit bring a charge? If transport is offered, is it totally free within a specific radius on particular days, or constantly billed per trip?
Insurance and advantages communicate with private pay in complicated ways. Standard Medicare does not pay for space and board in assisted living or memory care. It does cover eligible proficient services like treatment or hospice, no matter where the beneficiary resides. Long-term care insurance coverage may compensate a part of costs, but policies vary extensively. Veterans and making it through spouses might qualify for Help and Attendance benefits, which can balance out month-to-month fees. State Medicaid programs sometimes fund services in assisted living or memory care through waivers, but gain access to and waitlists depend upon geography and medical criteria.
How to examine a community beyond the tour
Tours are polished. Real life unfolds on Tuesday at 7 a.m. during a heavy care block, or at 8 p.m. when supper runs late and two locals require aid at once. Visit at various times. Listen for the tone of personnel voices and the way they talk to homeowners. Watch for how long a call light remains lit. Ask whether you can sign up with a meal. Taste the food, and not simply on an unique tasting day.


The activity calendar can misguide if it is aspirational rather than real. Stop by during a scheduled program and see who participates in. Are quieter locals participated in one-to-one moments, or are they left in front of a tv while an activity director leads a video game for extroverts? Range matters: music, motion, art, faith-based options, brain physical fitness, and unstructured time for those who prefer little groups.
On the medical side, ask how often care strategies are upgraded and who gets involved. The best strategies are collective, reflecting household insight about regimens, convenience objects, and long-lasting preferences. That well-worn cardigan or a little ritual at bedtime can make a new location seem like home.
Planning for development and preventing disruptive moves
Health changes gradually. A community that fits today should be able to support tomorrow, at least within a reasonable range. Ask what occurs if walking decreases, incontinence increases, or cognition worsens. Can the resident include care services in location, or would they require to transfer to a various apartment or system? Mixed-campus communities, where assisted living and memory care sit actions apart, make transitions smoother. Staff can float familiar faces, and families keep one address.
I think about the Harrisons, who moved into a one-bedroom in assisted living together. Mrs. Harrison delighted in the book club and knitting circle. Mr. Harrison had moderate cognitive disability that advanced. A year later, he moved to the memory care neighborhood down the hall. They ate breakfast together most early mornings and invested afternoons in their chosen areas. Their marriage rhythms continued, supported rather than eliminated by the structure layout.
When staying home still makes sense
Assisted living and memory care are not the only responses. With the ideal mix of home care, adult day programs, and innovation, some individuals thrive in your home longer than expected. Adult day programs can provide socializing, meals, and supervision for 6 to 8 hours a day, providing family caretakers time to work or rest. At home aides assist with bathing and respite, and a visiting nurse handles medications and wounds. The tipping point frequently comes when nights are hazardous, when two-person transfers are needed routinely, or when a caregiver's health is breaking under the stress. That is not failure. It is a truthful acknowledgment of human limits.
Financially, home care expenses accumulate quickly, particularly for over night protection. In lots of markets, 24-hour home care surpasses the regular monthly expense of assisted living or memory care by a large margin. The break-even analysis must consist of utilities, food, home maintenance, and the intangible expenses of caretaker burnout.
A brief choice guide to match requirements and settings
- Choose assisted living when a person is mainly independent, needs predictable help with day-to-day tasks, gain from meals and social structure, and remains safe without constant supervision. Choose memory care when dementia drives life, security needs protected doors and trained personnel, habits need ongoing redirection, or a busy environment regularly raises anxiety. Use respite care to check the fit, recuperate from disease, or give family caregivers a reliable break without long commitments. Prioritize communities with strong training, stable staffing, and clear care level criteria over simply cosmetic features. Plan for development so that services can increase without a disruptive relocation, and align financial resources with practical, year-over-year costs.
What families typically regret, and what they seldom do
Regrets rarely center on choosing the second-best wallpaper. They center on waiting too long, moving throughout a crisis, or choosing a neighborhood without comprehending how care levels adjust. Households nearly never ever be sorry for visiting at odd hours, asking difficult questions, and insisting on introductions to the real group who will supply care. They rarely are sorry for utilizing respite care to make decisions from observation rather than from fear. And they hardly ever are sorry for paying a bit more for a location where staff look them in the eye, call residents by name, and deal with little minutes as the heart of the work.
Assisted living and memory care can protect autonomy and meaning in a stage of life that should have more than safety alone. The best level of care is not a label, it is a match between an individual's needs and an environment created to meet them. You will understand you are close when your loved one's shoulders drop a little, when meals occur without triggering, when nights end up being predictable, and when you as a caretaker sleep through the first night without jolting awake to listen for footsteps in the hall.
The choice is weighty, but it does not have to be lonesome. Bring a note pad, invite another set of ears to the tour, and keep your compass set on life. The best fit shows itself in normal minutes: a caretaker kneeling to make eye contact, a resident smiling during a familiar song, a tidy bathroom at the end of a busy morning. These are the signs that the level of care is not just scored on a chart, however lived well, one day at a time.
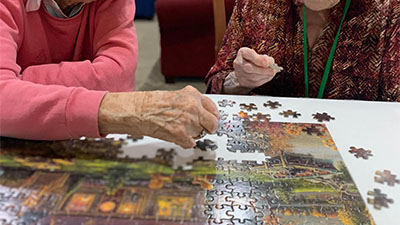
BeeHive Homes of Enchanted Hills provides assisted living care
BeeHive Homes of Enchanted Hills provides memory care services
BeeHive Homes of Enchanted Hills provides respite care services
BeeHive Homes of Enchanted Hills supports assistance with bathing and grooming
BeeHive Homes of Enchanted Hills offers private bedrooms with private bathrooms
BeeHive Homes of Enchanted Hills provides medication monitoring and documentation
BeeHive Homes of Enchanted Hills serves dietitian-approved meals
BeeHive Homes of Enchanted Hills provides housekeeping services
BeeHive Homes of Enchanted Hills provides laundry services
BeeHive Homes of Enchanted Hills offers community dining and social engagement activities
BeeHive Homes of Enchanted Hills features life enrichment activities
BeeHive Homes of Enchanted Hills supports personal care assistance during meals and daily routines
BeeHive Homes of Enchanted Hills promotes frequent physical and mental exercise opportunities
BeeHive Homes of Enchanted Hills provides a home-like residential environment
BeeHive Homes of Enchanted Hills creates customized care plans as residents’ needs change
BeeHive Homes of Enchanted Hills assesses individual resident care needs
BeeHive Homes of Enchanted Hills accepts private pay and long-term care insurance
BeeHive Homes of Enchanted Hills assists qualified veterans with Aid and Attendance benefits
BeeHive Homes of Enchanted Hills encourages meaningful resident-to-staff relationships
BeeHive Homes of Enchanted Hills delivers compassionate, attentive senior care focused on dignity and comfort
BeeHive Homes of Enchanted Hills has a phone number of (505) 221-6400
BeeHive Homes of Enchanted Hills has an address of 6336 Enchanted Hills Blvd NE, Rio Rancho, NM 87144
BeeHive Homes of Enchanted Hills has a website https://beehivehomes.com/locations/enchanted-hills/
BeeHive Homes of Enchanted Hills has Google Maps listing https://maps.app.goo.gl/5LqAWwumxTEeaW5p7
BeeHive Homes of Enchanted Hills has Instagram page https://www.instagram.com/beehivehomesriorancho/
BeeHive Homes of Enchanted Hills has an YouTube page https://www.youtube.com/@WelcomeHomeBeeHiveHomes
BeeHive Homes of Enchanted Hills won Top Assisted Living Homes 2025
BeeHive Homes of Enchanted Hills earned Best Customer Service Award 2024
BeeHive Homes of Enchanted Hills placed 1st for Senior Living Communities 2025
People Also Ask about BeeHive Homes of Enchanted Hills
What is BeeHive Homes of Enchanted Hills Living monthly room rate?
The rate depends on the level of care that is needed. We do a pre-admission evaluation for each resident to determine the level of care needed. The monthly rate is based on this evaluation. There are no hidden costs or fees
Can residents stay in BeeHive Homes until the end of their life?
Usually yes. There are exceptions, such as when there are safety issues with the resident, or they need 24 hour skilled nursing services
Do we have a nurse on staff?
No, but each BeeHive Home has a consulting Nurse available 24 – 7. if nursing services are needed, a doctor can order home health to come into the home
What are BeeHive Homes’ visiting hours?
Visiting hours are adjusted to accommodate the families and the resident’s needs… just not too early or too late
Do we have couple’s rooms available?
Yes, each home has rooms designed to accommodate couples. Please ask about the availability of these rooms
Where is BeeHive Homes of Enchanted Hills located?
BeeHive Homes of Enchanted Hills is conveniently located at 6336 Enchanted Hills Blvd NE, Rio Rancho, NM 87144. You can easily find directions on Google Maps or call at (505) 221-6400 Monday through Sunday 9:00am to 5:00pm
How can I contact BeeHive Homes of Enchanted Hills?
You can contact BeeHive Homes of Enchanted Hills by phone at: (505) 221-6400, visit their website at https://beehivehomes.com/locations/enchanted-hills/ or connect on social media via Instagram TikTok or YouTube
Conveniently located near Beehive Homes of Enchanted Hills Rio Rancho Premiere a great movie theater with full food & drink menu. Catch a movie and enjoy some great food while you wait.